Infected Diabetic Foot Ulcers: When Surgery Is Needed and How It Can Save Your Foot
Diabetic foot ulcers are one of the most serious complications of diabetes, especially when they become infected. An Infected Diabetic Foot can progress rapidly, leading to deep tissue damage, bone involvement, and even limb loss if not treated promptly. While early-stage ulcers may respond to medication and wound care, advanced infections often require surgical intervention. Understanding when surgery is needed and how it helps is crucial for preventing long-term disability and preserving foot function.
What Makes a Diabetic Foot Ulcer Infected?
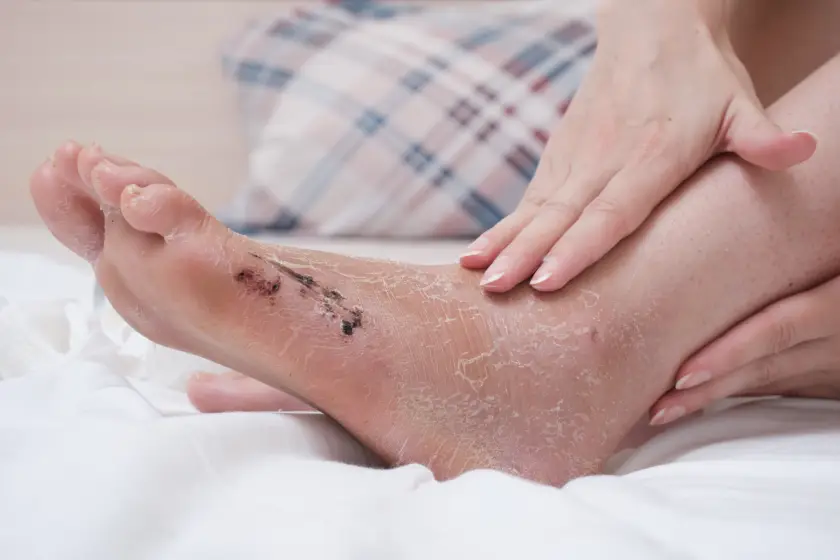
An ulcer becomes infected when bacteria enter through an open wound and multiply faster than the body can control. Diabetic foot ulcer infection is more common due to reduced immunity, poor blood circulation, and nerve damage that delays detection of injuries. Signs of an infected diabetic foot ulcer include redness, swelling, warmth, pus discharge, foul odor, increasing pain, and fever. In severe cases, infection may spread to deeper tissues or bone, making conservative diabetic foot ulcer treatment ineffective.
When Is Surgery Needed for Infected Diabetic Foot Ulcers?
Surgery is recommended when infection does not respond to antibiotics, wound care, or offloading methods. An Infected Diabetic Foot may require surgical intervention if there is dead tissue, abscess formation, spreading infection, or bone involvement. Delayed treatment can allow infection to advance rapidly, increasing the risk of amputation. Timely diabetic foot ulcer surgery aims to control infection, remove damaged tissue, and promote healing while preserving as much healthy tissue as possible.
Surgical Treatment Options for Infected Diabetic Foot Ulcers
Surgical management is tailored to the severity and extent of infection. Procedures may include debridement to remove infected and dead tissue, drainage of abscesses, correction of deformities causing pressure points, or bone surgery in cases of osteomyelitis. In advanced cases, partial amputations may be necessary to stop the spread of infection. These procedures form a critical part of comprehensive Diabetic foot infection treatment, often combined with antibiotics and wound care to achieve optimal outcomes.
What to Expect Before Infected Diabetic Foot Surgery
Before surgery, patients undergo a detailed evaluation, including blood tests, imaging studies, and wound assessment to determine the extent of infection. Blood sugar levels are carefully controlled, as poor glycemic management can delay healing. The surgical plan is explained in detail, including risks and expected outcomes. Preparing for diabetic foot ulcer surgery also involves optimizing circulation, managing existing medical conditions, and educating the patient about post-operative care.
How Infected Diabetic Foot Surgery Helps Save the Foot
Surgery plays a vital role in limb preservation by removing the source of infection and preventing its spread. By eliminating dead tissue and reducing bacterial load, Infected Diabetic Foot surgery creates a healthier environment for healing. Corrective procedures also help redistribute pressure, reducing the risk of ulcer recurrence. When performed early, surgical intervention significantly improves the chances of saving the foot and avoiding major amputation, making it a cornerstone of advanced diabetic foot ulcer treatment .
Infected Diabetic Foot Post-Surgery Care & Recovery
Recovery after surgery requires close monitoring and strict adherence to medical advice. Wound care, antibiotics, offloading, and regular follow-ups are essential to ensure proper healing. Patients are advised to limit weight-bearing initially and gradually resume activity as healing progresses. Long-term recovery also includes lifestyle changes, custom footwear , and continued Diabetic foot infection treatment to prevent recurrence. With proper care, many patients regain mobility and avoid further complications.
Conclusion
An Infected Diabetic Foot is a medical emergency that requires prompt and appropriate treatment. While early-stage ulcers may heal with conservative care, advanced infections often need surgical intervention to prevent limb loss. Modern diabetic foot ulcer surgery focuses on infection control, tissue preservation, and functional recovery. Early diagnosis, timely surgery, and comprehensive post-operative care together offer the best chance to save the foot and improve the quality of life for diabetic patients.
FAQs
When does an infected diabetic foot ulcer require surgery?
Surgery is required when infection does not improve with antibiotics and wound care, or when there is dead tissue, abscess formation, spreading infection, or bone involvement. In such cases, delaying surgical intervention can allow the infection to worsen and increase the risk of serious complications, including limb loss.
What types of surgeries are performed for infected diabetic foot ulcers?
Procedures may include debridement to remove infected or dead tissue, abscess drainage to control deep infection, bone surgery when infection reaches the bone, corrective procedures to reduce pressure points, or partial amputation in advanced cases. The choice of surgery depends on the severity and extent of the infection.
Can surgery help save the foot and avoid amputation?
Yes, timely diabetic foot ulcer surgery can control infection early, prevent its spread to healthy tissues, and significantly reduce the risk of major amputation. Early surgical treatment often preserves foot structure and improves long-term mobility.
What should a patient expect before diabetic foot surgery?
Patients undergo a detailed evaluation that includes infection assessment, imaging studies, and blood tests. Blood sugar levels are carefully optimized to support healing, and the surgical plan is explained clearly. Patients are also counseled about the procedure, possible outcomes, and post-surgery care requirements.
How long does recovery take after surgery for an infected diabetic foot ulcer?
Recovery varies based on the severity of infection and the type of procedure performed. Most patients require several weeks of wound care, restricted weight-bearing, and regular follow-up visits to ensure proper healing and prevent recurrence.